If you’ve noticed brown spots or markings on your skin lately, you may be wondering what they are and if you should be concerned. These brownish spots are often due to hemosiderin staining. In this comprehensive guide, we’ll cover everything you need to know about it like:
- What are the Hemosiderin staining causes?
- Is hemosiderin staining treatment necessary
- Is hemosiderin staining dangerous
What is Hemosiderin Staining?
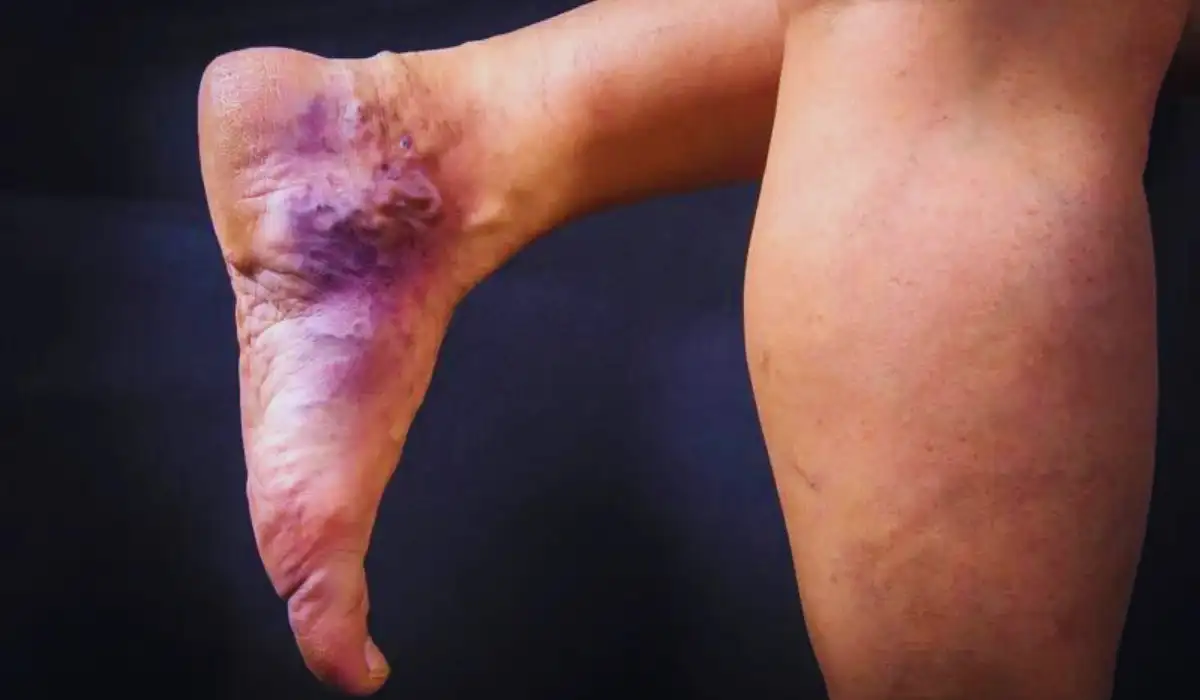
Hemosiderin staining refers to a condition where excess iron in the form of Hemosiderin gets deposited under the skin. This will lead to the formation of brown, red, yellow, or blue markings or spots on the skin.
Hemosiderin is an iron-rich compound that the body stores internally to regulate iron levels. When blood vessels are damaged from injury, surgery, or other causes, hemosiderin can leak out and become trapped under the skin at the site of the damage. This results in stain-like skin discoloration we call hemosiderin staining. So, is hemosiderin staining dangerous?
While unsightly, hemosiderin staining is generally harmless. But what causes these frustrating spots?
What are the Hemosiderin Staining Causes?
There are several potential hemosiderin staining causes on the skin,
- Bruising/Internal Bleeding: Bruises happen when blood vessels rupture under the skin, allowing blood and iron to pool inside tissues. As the bruise fades, the leftover iron can oxidize into hemosiderin deposits.
- Surgery/Medical Procedures: Surgical incisions and other invasive medical procedures can damage blood vessels enough to trigger localized bleeding/bruising.
- Trauma/Injuries: Any blunt force injuries that rupture blood vessels may cause bleeding/bruising and subsequent skin discoloration from hemosiderin.
- Vein Damage: Faulty veins often leak blood internally, allowing iron to build up. This is why hemosiderin staining frequently occurs on the lower legs.
Is Hemosiderin Staining Dangerous?
When one hears about hemosiderin staining they will naturally start to wonder, is hemosiderin staining dangerous? In most cases, hemosiderin skin staining is harmless and poses no medical threat or risks.
The discoloration is primarily a cosmetic nuisance. However, extensive bruising and bleeding that leads to substantial hemosiderin buildup can theoretically damage tissues and organs if left unchecked. But for typical minor skin staining, there is very little cause for health concerns.
Hemosiderin Staining Symptoms
The primary symptom of hemosiderin staining is skin discoloration. Markings and spots may appear in different shades of brown, red, yellow, purple, or blue. The color variation depends on how long ago the bleeding occurred and how deep under the skin the hemosiderin iron settled.
Staining can occur anywhere on the body but is most prevalent on the,
- Legs: Lower legs around the ankles and calves often develop hemosiderin staining due to chronic venous insufficiency and related vein/capillary damage.
- Torso: Staining frequently appears on the breast, chest, stomach, and back due to trauma, surgery, or unknown internal bleeding episodes.
- Face: The fragile capillaries around the eyes and cheeks commonly rupture leading to facial hemosiderosis.
In addition to skin discoloration, hemosiderin deposits may appear slightly raised or uneven compared to the surrounding skin. They often gradually fade over many months.
Hemosiderin Staining Treatment and Removal
While hemosiderin skin staining can take a year or longer to fully resolve, the below-listed hemosiderin staining treatment plans can speed up their fading,
- Vitamin C: When applied topically or taken orally, vitamin C helps boost collagen production and skin cell turnover to help clear discoloration.
- Retinoids: Retinoids increase cell regeneration to expedite staining removal. Non-prescription retinols are gentler but still effective.
- AHAs: Alpha hydroxy acids like glycolic or lactic acid promote exfoliation and fading of stained skin cells.
- Laser Resurfacing Procedures: Dermatologists can use laser energy to destroy stained skin cells and trigger the regeneration of clear new cells.
- Microdermabrasion/Chemical Peels: These professionally administered treatments remove stained tissue layers so unblemished cells rise to the surface.
- Makeup/Concealer: Cosmetic products like color correction creams and concealers effectively hide skin discoloration temporarily.
While waiting for hemosiderin staining to fade, you can talk to your doctor about adding iron supplements or performing phlebotomy to bring down excess iron levels in chronic cases. But for most people with minor skin staining, just having patience for the spots to slowly clear is enough.
Conclusion
In closing, hemosiderin skin staining refers to harmless discoloration caused by bleeding and iron deposits under the skin’s surface. Staining frequently occurs after surgeries, medical procedures, or blunt force trauma that ruptures blood vessels.
Lower legs are particularly prone to hemosiderin spots due to chronic vein damage and blood pooling.
While unsightly and frustrating, typical minor cases of hemosiderin skin discoloration pose very few health issues. You don’t usually need medical treatment.
Fortunately, there are several home options you can try to help reduce the appearance of staining faster – including vitamin C, retinoids, AHAs, and diligent makeup coverage. Professional procedures like laser treatments can also expedite the removal of stubborn spots.
In the end, as frustrating as it seems when those stain spots first appear, try to be patient. With time and a little TLC for your skin, those marks will gradually but surely fade. And if they still bother you after a year or so, your dermatologist can recommend next-step procedures tailored to your unique case.
Does lingering hemosiderin staining frustrate you? What remedies have (or haven’t) worked to reduce your spots? Let us know in the comments!
Reference
- HamiltonHK, et al. (2014). Successful treatment of disfiguring hemosiderin-containinghyperpigmentation with the Q-switched 650-nm wavelength laser. DOI:
https://doi.org/10.1001/jamadermatol.2014.1838

